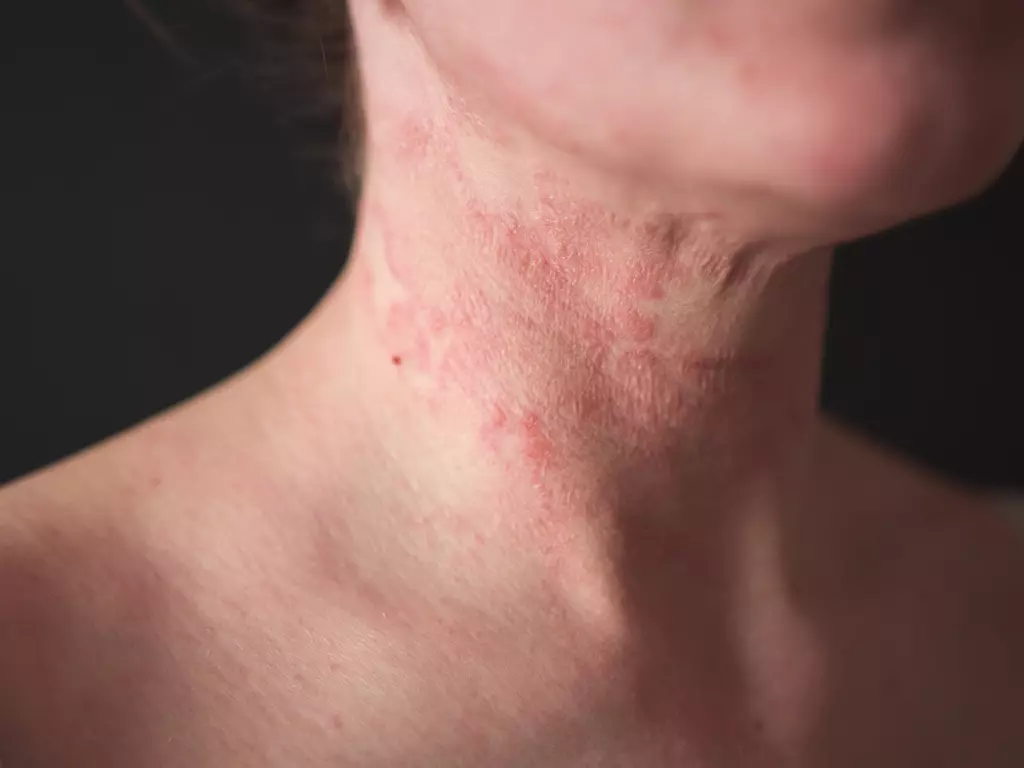
Eczema is a chronic inflammatory skin condition characterized by dryness, irritation, and recurrent flare-ups, significantly affecting daily comfort and skin integrity. Because symptoms are often triggered by environmental factors, allergens, stress, or skincare products, proactive management is necessary. Reducing the frequency and severity of flare-ups requires a combination of consistent skincare practices, trigger identification, and appropriate medical guidance.
Strengthen the Skin Barrier Daily
Your skin’s natural barrier protects it from irritants and allergens, but eczema weakens this protection. Rebuilding and maintaining this barrier is necessary to prevent flare-ups. Moisturize your skin at least twice daily with a thick, fragrance-free cream or ointment. Apply moisturizer immediately after bathing to lock in moisture while your skin is still damp.
Shorter, lukewarm baths or showers are better than long, hot ones, which strip away natural oils. Use gentle, fragrance-free cleansers specifically designed for sensitive skin, and pat your skin dry with a towel instead of rubbing it. Humidity also affects skin health. During dry months, use a humidifier to add moisture to the air and prevent your skin from drying out.
Identify and Eliminate Eczema Triggers
Eczema triggers are different for everyone. Identifying yours is key to managing flare-ups. Common triggers include fabrics, soaps, pet dander, pollen, and foods. To find your triggers, keep a symptom diary. Note what you ate, the products you used, and your environment when symptoms appear. Over time, you will see patterns that help you pinpoint what causes your flare-ups.
Once you know your triggers, you are able to avoid them. Choose cotton fabrics over wool or synthetics. Use hypoallergenic laundry detergents and avoid fabric softeners. They sometimes leave irritating residues on clothes. If you suspect food triggers, talk to your doctor. Common food triggers include dairy, eggs, nuts, and soy. Only eliminate foods with medical guidance.
Manage Stress and Environment
Stress is a powerful trigger for eczema flare-ups. It weakens your immune system and increases inflammation. Managing stress reduces the frequency and severity of your outbreaks. Try stress-reduction techniques like deep breathing, meditation, or yoga. Regular physical activity also helps lower stress levels. Make sure you get enough sleep each night. Lack of rest can worsen both stress and eczema.
Environmental factors also trigger flare-ups. These include extreme temperatures, low humidity, and allergens. Dress in layers to adjust to temperature changes. Avoid overheating or excessive sweating when possible. Keep your living space clean. This reduces your exposure to dust mites and pet dander. Wash your bedding weekly in hot water. You might also use allergen-proof pillow and mattress covers.
Use Preventive Early Treatments
Medical treatments do help manage eczema and prevent flare-ups. It’s best to work with your dermatologist to create a plan for your needs. Topical corticosteroids reduce inflammation during flare-ups. Use them as directed by your doctor to avoid side effects, such as skin thinning. Non-steroidal topical medications are an alternative for sensitive areas. These include calcineurin inhibitors for the face and eyelids.
For severe cases, your doctor may suggest phototherapy. This uses controlled light to reduce symptoms. Newer biologic medications are another option. They target specific parts of the immune system. Don’t wait for a severe flare-up to seek treatment. Early intervention does prevent symptoms from worsening. This helps you maintain better control over your condition.
Schedule an Eczema Treatment Consultation
Managing eczema requires a consistent approach that combines daily skin care, trigger avoidance, stress management, and medical treatment. When you strengthen your skin barrier, identify your personal triggers, and work closely with a dermatologist, you can reduce flare-ups and enjoy healthier skin. If you’re struggling to control your eczema, schedule an appointment with a board-certified dermatologist for an assessment and an effective treatment plan to find the relief you deserve.